PinPointe ™ FootLaser ™
Say goodbye to embarrassing toenail fungus
The PinPointe™ FootLaser™ is the first clinically proven laser device for the treatment of patients with onychomycosis, or nail fungus.
what is toenail fungus
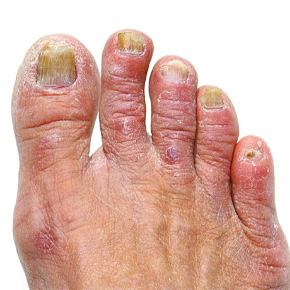
Toenail fungus is characterised by thick, unsightly, discoloured nails. Fungus-infected toenails can be irritating, embarrassing and painful. Leaving a fungal infection untreated can result in it spreading to other toenails, the skin on the feet and even the fingernails. Severe cases can impair one’s ability to walk or lead to painful ingrown toenails.
treatment for fungal nails
Safe and effective, this in-office treatment is pain free, has no harmful side effects, and typically takes only about 30-minutes to complete, turning your discoloured and disfigured nails into clearer, healthier looking nails.
It’s important to seek care when you notice signs of infection.
For years, the only treatments available for toenail fungus were topical and oral medications, or removal of the nail. Typically, the medications were largely ineffective and removal of the nail plate was painful and debilitating.
However, a new breakthrough in technology is making it possible to get rid of your nail fungus fast – a new procedure known as PinPointe™ FootLaser™. The new, patented laser technology treats nail fungus safely and quickly with no drugs, no anaesthesia and no pain.
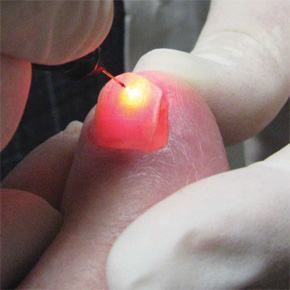
How PinPointe™ FootLaser™ works
The PinPointe™ FootLaser™ is specially designed to penetrate your toenail, vaporising the fungus embedded deep in your nail bed. The powerful laser beam targets the infection only and has no effect on surrounding healthy tissue.
The impact of unsightly nail fungus
Toenail fungus is a common condition that disfigures and sometimes destroys the nail. Fungi thrive in the warm, dark, moist environments – such as a shoe. As the fungus grows, it feeds on the nail plate, destroying and disfiguring it.
The treatment of nail infection is difficult because the infection is under and inside of the nail, which makes it hard for other treatments to reach and destroy the infection.
Only the PinPointe™ FootLaser™ is designed specifically to treat the major symptoms of discoloured and unsightly nails.

Talk to the footinjuryclinic about treatment options currently available for nail infection to determine which is the right treatment for you.
Treatment plan:
PinPointe ™ FootLaser ™
Benefits
1. Effective in treating nail infections – Most patients receive some improvement in 3, 6, 9 and/or 12 months after one treatment session
2. New nail grows out with no signs of infection
3. No significant adverse effects
Risks
1. Not effective in all patients
2. Final result seen after nail grows out (4-12 months)
3. Usual side effect: feeling of warmth (only during treatment)
4. Rare side effects:
– Discoloration/burn marks on surface of the nail
– Slight or mild pain (only during treatment)
– Redness of the treated skin around the nail (lasting 24-72 hours)
– Slight swelling of the treated skin around the nail (lasting 24-72 hours)
5. Rare laser effect:
– Sometimes the laser creates ‘sparks’ on the surface of the nail – this does not cause any problems
6. Extremely rare laser effects (did not occur during clinical studies):
– Blistering of the treated skin around the nail
– Scarring of the treated skin around the nail
Oral Drugs
Benefits
1. Effective in treating nail infections
2. New nail grows out with no signs of infection
Risks
1. Drug must be taken for 6-12 weeks
2. Not effective in all patients
3. Not recommended in some patients with poor health
4. Final result seen after nail grows out (4-12 months)
5. Drug side effects: headache, diarrhoea, upset stomach, skin rash (allergic reaction to drug)
6. Serious drug side effects: risk of liver damage and heart failure (weekly blood testing may be required to monitor liver/heart function)
Topical Drugs
Benefits
1. Has some effectiveness
2. New nail grows out without signs of infection
3. No significant adverse effects
Risks
1. Drug must be applied to nails daily for a long period
2. Not effective in all patients as the drug cannot pass through the nail to reach the infection under the nail
Tips to avoid irritating toenail fungus:
- Practice good hygiene and inspect feet and toes regularly
- Try not to injure your nail by cutting it too short, as trauma to the nail may lead to infection
- Wear moisture absorbing socks
- Wear dry, proper-fitting shoes that allow air to circulate around your feet
- Wear shower sandals when you are at a public pool or shower
Frequently asked questions about toenail fungus and laser treatment:
Q. How do I know if I have toenail fungus?
A. The most common signs of toenail fungus are:
- Discoloration, such as yellowish, brown and or grayish changes in portions of the nail or the entire nail plate
- Thickness and deforming of the nail plate
- Either a crumbling nail or a very firm and rigid nail plate
- Unpleasant odor
- Debris under the toenail
Q. What exactly is nail fungus and where does it come from?
A. The medical terminology for nail fungus is onychomycosis. A nail fungus is a microorganism that could be one of several invading parasites in the nail and nail bed (the tissue in which the nail plate rests). The invading parasites contaminate all layers of the nail anatomy, including the nail itself, the nail bed, the cuticle and the nail growth centre.
Q. How do you get toenail fungus? Is it contagious?
A. There are several sources of fungal and bacterial nail infections which can be contagious. A fungus is a living organism that can be transmitted from one person to another. It can be transmitted in places like shower stalls, locker rooms, dirty floors and old shoes or by wearing someone else’s shoes that has the infection. The fungus also can be spread from one of your toenails to your another one of your toenails. It is possible for the infection to be spread from pedicures at nail salons as the fungus can be transmitted through nail polish and instruments that are not properly sterilised.
Injury is another cause of nail fungus. If your toenail has been injured by stubbing it or by accidentally dropping an object on it or even by consistently wearing tight-fitting shoes, the natural barrier of the skin around the nail becomes compromised and the fungus can easily penetrate under the nail.
Q. Is toenail fungus more common in men or women?
A. We tend to see more men affected because men wear more closed-toe shoes than women and usually have sweatier feet. Wearing the same infected shoes also increases the chance of constantly re-infecting your skin and nails. This is one of the reasons why it is important to disinfect your shoes following laser treatment, especially for men.
Q. How does the laser work?
A. The laser produces multiple light wave lengths that seek out the fungal cells. The laser only targets the fungal cells and does not harm or destroy the skin or tissue surrounding nail. The laser light penetrates through the nail to the diseased cells on the nail bed and roots where the fungal infection resides.
Q. Does the laser treatment procedure hurt?
A. There is no pain during laser treatment. Since the treatment is not painful, no local anaesthesia or injections are necessary. If the nail plate is loose, sometimes during debridement of the nail prior to the treatment you may have minimal discomfort. Most patients describe the laser treatment procedure as being comfortable with a quick, small pinch at the end. Immediately following the procedure, your nails may feel warm for a few minutes.
Q. How long does the laser treatment take?
A. The actual laser treatment process takes about 20 to 30 minutes if treating all ten toes. To prepare your nails for the procedure, our podiatrist will perform a professional medical pedicure utilising sterilised equipment. This process is painless and includes thinning the toenails to allow the laser to more effectively penetrate the nails during the treatment.
Q. Are there any side effects from the laser treatment?
A. There are no side effects from the treatment. There are no post-treatment complications or adverse reactions from the laser nail treatment. In addition, patients can resume normal activities immediately.
Q. May I continue to get pedicures and polish my nails during the recovery period?
A. Yes. You can apply nail polish.
Q. How long will it take for me to see results?
A. Most individuals begin to see results after approximately two to three months depending on the severity and amount of nail that is involved. Not all nails grow at the same rate so clearing varies from patient to patient and nail to nail depending upon the depth of the fungal infection.
During the growth period following the treatment, the new nail grows from the cuticle and pushes the infected nail out toward the end of the toe. Normal trimming and nail filing should occur during this standard nail-growth phase so that the old, diseased nail is trimmed off. At each follow-up laser treatment, the podiatrist will trim and mechanically thin the nail plate for faster results. We do know that patients who have had the disease for many years may require additional laser treatments. No two patients act identically in how long the overall treatment will take to show results. The results also may vary due to previous injury or underlying disease that may have influenced the nail infection and deformity. Some patients may require a biannual maintenance program that includes a sterile medical debridement and an additional laser treatment. Our podiatrist will advise you as you progress throughout the treatment cycle.
Q. What is the chance of the infection returning?
A. There is always a chance of re-infection if you are exposed to a new fungal infection; however, we have seen very few re-infections. We will provide you with important information on care and prevention for a lifetime of fungus-free feet. As stated earlier, chronic long-term nail infections may take longer to resolve.
Q. Can I have this procedure preformed if I am a diabetic?
A. With every diabetic there is the possibility of vascular disease or nerve disease called peripheral neuropathy. Diabetics are in danger of infections due to either advanced vascular disease or nerve disease due to thick and contaminated nail plates from the presence of a fungal infection. When the nails become thick due to the fungus, the thick nail plate can cause excessive pressure under the nail plate on the nail bed. The constant pressure of the shoe breaks down the tissue and either an ulcer can form or a collection of blood called a subungual haematoma or “blood blister” can form. Both of these are dangerous for a diabetic and can cause an infection if untreated. In the case of a diabetic with neuropathy, which is a reduction in feeling in the toes and feet, this infection may worsen and create an abscess that can then infiltrate the bone. Once this occurs, the podiatrist would need to remove the nail.
We encourage diabetics who are capable of having this procedure to either have the laser decontamination of the nails or routine foot care by a podiatrist for manual debridement to protect themselves from complications. In summary, we encourage diabetic patients to have this procedure if all of their medical findings are within the normal treatable parameters.
Q. Is this treatment covered by my Health cover?
A. Unfortunately, no. At this time, health cover plans consider this treatment as cosmetic and thus do not cover this type of procedure.