Plantar Fasciitis Sydney
The term plantar fasciitis describes an injury in which the ligament which runs from your heel to the ball of your foot becomes damaged, inflamed and painful. This condition is commonly caused by abnormal stress along your plantar fascia at its attachment to the heel bone. Abnormal stress is often caused by your foot excessively rolling in at the ankle, a condition known as pronation. Stress can also result from a bruise or injury incurred whilst exercising, wearing poor quality shoes or being overweight, all of which can overload your plantar fascia.
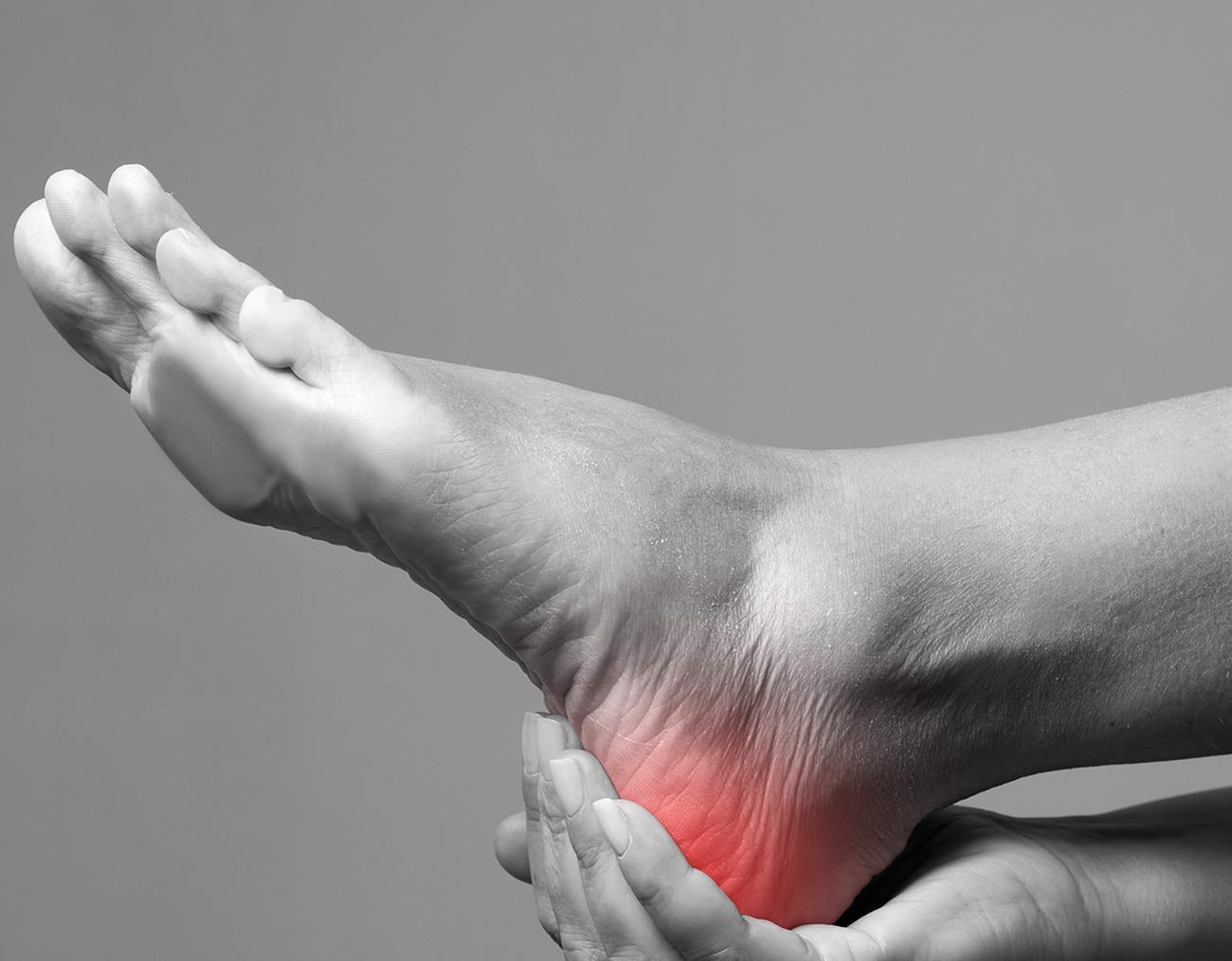
symptoms of plantar fasciitis
Plantar fasciitis causes a number of symptoms that include:
- Sharp, stabbing pain on the bottom or side of the heel or in the arch of the foot.
- Pain that is worse in the morning or after any period of inactivity. As you begin to move around, the pain level usually improves.
- Pain that gets worse after a prolonged period of standing, walking, or running.
- Pain that can last for several weeks or months and can range from mild to severe.

screening and diagnosis
We usually diagnose plantar fasciitis by asking you about your symptoms and physically examining your foot. At the footinjuryclinic we have state of the art video gait analysis and pressure fluoroscopes which we use in aiding our diagnosis. We may order an imaging study, such as an X-ray, if we suspect that your symptoms may be caused by another condition, such as a stress fracture, but this is rare.
who gets plantar fasciitis
There are a number of factors that can increase the likelihood that you will develop plantar fasciitis including:
- Excess weight
- Specific sports activities
Activities that put significant pressure on your foot and require it to stretch repeatedly increase your risk. These activities include running, walking long distances, jumping, tennis, beach running and aerobics. - Age
Middle-aged people, between 40 and 60 years old are more likely to develop plantar fasciitis. - Abnormal foot mechanics
Flat feet or high arches can affect the way that pressure is distributed across your foot ,placing additional stress on the plantar fascia. - Tight Achilles tendon and excessive flattening of your feet (pronation)
The Achilles tendon links the calf muscle to the back of the heel. A tight calf muscle and Achilles tendon can cause your foot to flatten further, placing additional stress on the plantar fascia. - Standing all day
Standing or walking on hard floors for a long time increases the load on your plantar fascia. - Inadequate footwear
Excessively flat shoes that do not support your arch leave the plantar fascia unprotected. A shoe with a medium heel can heighten the arch and decrease stress on the plantar fascia. - Sudden change in activity
Beginning an exercise program , such as high-impact aerobics, after a period of inactivity can overload the structures in your foot. Similarly, changing your running surface from grass to road can affect your plantar fascia.
prevention of plantar fasciitis
There are a number of things you can do to protect your feet and prevent injury to your plantar fascia:
- Wear supportive shoes
We recommend running shoes or “pro” walking shoes. It’s a good idea to wear these when you are running or walking a long distance or when you will be on your feet for an extended period of time. - Wear shoes with slightly higher heels
A moderate heel can shorten the arch, reduce stress on the plantar fascia, and lead to a reduction of pain. At the footinjuryclinic we recommend a ladies heel of around 2.5cm. - Do not walk barefoot
Even at home when suffering from plantar fasciitis. - Lose weight
Talk to your personal doctor, trainer or dietician. - Stretch
It is important to warm up before you exercise. Stretching your calf muscles will help protect your Achilles tendon, which in turn will ensure that your feet land correctly during walking and running.
treatment
It may take 3 to 12 months for your plantar fascia to heal completely. We recommend using a number of treatment approaches simultaneously, home and medical. It is important that you continue treatment until you have been pain-free for at least 3 months.
- Rest
Rest your foot for 2 to 6 weeks. Stand, walk, or run less. - Change your activities
While your foot is resting, try exercise that does not stretch your arch, like swimming or cycling. - Choose footwear that supports your foot
Shoes and devices that support your foot can help protect your plantar fascia and allow it to heal. We recommend a combination of the following footwear and devices:
– Supportive shoes
Wear shoes with good arch and heel support. A higher heel may also help. Avoid standing or walking barefoot or in unsupportive shoes like slippers or sandals.
– Arch supports
Wearing arch supports inside your shoes reduces strain on the plantar fascia. We recommend the Orthema EVA molded orthoses.
– Use over-the-counter pain relievers
Over-the-counter (OTC) nonsteroidal anti-inflammatory drugs (NSAIDs), such as Ibuprofen or Volatren can help manage your pain or discomfort. OTC NSAIDs are effective pain relievers that can be used if you have no health conditions that prevent you from taking them. Even though you do not need a prescription for OTC NSAIDs, you should be careful to consult the package so that you take the correct dose.Be aware that OTC NSAIDs can interact with other medicines you may be taking and cause problems for people with various medical conditions. These medications can help reduce the pain while your plantar fascia is healing. If they do not seem to be helping, do not continue taking them.
If you have a complex medical condition, are pregnant or trying to get pregnant, or have been taking OTC NSAIDs and they do not relieve your symptoms, please let us know so that we can recommend an alternative. Anti-inflammatory medication (if tolerated) and natural substances such as arnica may help reduce your pain and swelling. However, it is best to avoid anti-inflammatory drugs during the initial 48 to 72 hours when they may encourage additional bleeding. Most people can tolerate paracetamol as a pain reducing medication. - ice your foot
Massage the painful area with ice for 2 to 10 minutes , several times a day. A frozen water bottle can provide you with a ice foot roller that can simultaneously provide you with some gentle plantar fascia massage. - stretch
Stretch your calf muscles and Achilles tendon. It’s important to stretch before and after you exercise. We recommend that you warm up a little and then stretch at the beginning of your exercise program, if possible. footinjuryclinic recommended stretches FIC Stretches. - strapping/taping
Low Dye taping for the feet that can be performed by your podiatrist and taught to self application. - nonsurgical medical treatments
If the home treatment methods do not completely resolve your symptoms , we may recommend additional treatments that may include:
– Custom orthotic insoles
We recommend custom orthotic inserts that are made specifically for your foot. We use Orthema CAD/CAM digital technology in order to create these inserts.– Physiotherapy– Cortisone injections
We may recommend a cortisone injection to reduce inflammation and accompanying pain. Cortisone is a steroid that mimics natural hormones that reduce inflammation.



